Summary
Description
Unicameral bone cysts (UBC), also known as simple bone cysts, are lesions that consist of a fluid filled cavity lined by a thin membrane.
People and Age
It is found most commonly in children ages 5-20, but these lesions occasionally persist into adulthood.
Symptoms and Presentation
Most UBC's are asymptomatic and only present when a pathological fracture occurs. Some are discovered as incidental findings during an evaluation for an unrelated injury or condition.
Brief description of the xray
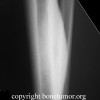
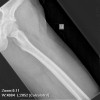
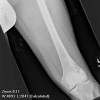
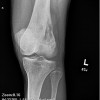
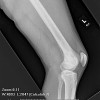
The lesion appears as a relatively symmetrical, well defined osteolytic area with a thin sclerotic margin.
Brief desc of tx
Closed treatment of the fracture is first priority. One to three percutaneous methyl prednisolone acetate injections at two month intervals have been sucessful at similar rates with a significantly less invasive procedure. The injections consist of 2-5ml of MPA with 2 needles introduced.
Complete Information on this Tumor
Introduction and Definition
Unicameral bone cysts (UBC), also known as simple bone cysts, are lesions that consist of a fluid filled cavity lined by a thin membrane. They are found in the metaphysis of long bones, with the most common site being the proximal humerus, followed by the proximal femur. "Active" cysts are located near the epiphysis (such as in the top two images), and as they move farther away (such as in the third image) as the child grows they become inactive. The lesion may be found in unusual sites such as the calcaneous and pelvis in patients more than 17 years old. The etiology of UBC's is unknown. It is possible the lesion is a reaction to trauma. The most popular theory is that local venous obstruction causes an increase in pressure which leads to reactive bone resorption. The cyst fluid contains prostaglandin and IL-IB which independently can cause bone resorption.
Incidence and Demographics
UBC's are found most commonly in children between the ages of ages 5 to 20 years old, and the ratio of male to female is 2:1.
Symptoms and Presentation
Most UBC's are asymptomatic and only present when a pathological fracture occurs.
X-Ray Appearance and Advanced Imaging Findings
The plain film is usually enough to make a diagnosis of a UBC, once the observer is thoroughly familiar with the appearance of this lesion. The lesion appears as a well defined osteolytic area with a thin sclerotic margin. It fills and perhaps slightly expands the juxta-epiphyseal metaphysis of the bone. The lesion is relatively symmetrical with respect to the midline axis of the bone. The lesion is not eccentric and does not break out through the cortex or form any extra osseous mass. There is no periosteal reaction visible unless there has been a previous fracture. A fragment of cortex that has fallen into a dependent position inside the cyst is known as the "fallen leaf" or "fallen fragment" sign. CT scan is not helpful unless the UBC is in the pelvis. MRI is also not useful unless it demonstrates fluid signals which are low signals on T1 weighted images and bright signal on T2 images. On bone scan, UBC's have light peripheral uptake with a cold center.
Laboratory Findings
There are no helpful laboratory tests for this tumor.
Histopathology findings
Microscopically, the UBC has a membrane made up of a layer of flattened or cuboidal cells that resemble endothelium. The cyst fluid resembles synovial fluid. If a fracture has occured, there may be a hemorrhage, granulation tissue, calcifications, or giant cells which may confuse the diagnosis.
Treatment Options for this Tumor
Treatment of UBC's can take several forms. The physician must be extremely confident of the diagnosis and should obtain a consultation if he or she does not see the lesions frequently. When the lesion presents with a pathological fracture, closed treatment of the fracture is the first priority. Sometimes the trauma and subsequent healing process of a pathological fracture can be enough to cause resolution of the UBC. One to three percutaneous methyl prednisolone acetate injections at two month intervals have been sucessful at similar rates with a significantly less invasive procedure. The injections consist of 2-5ml of MPA with 2 needles introduced into the cavity to reduce venous hemorrhage and to keep the medication in the lesion as much as possible.
Surgical treatment is sometimes necessary for lesions that are large or where the bone is weakened and pathological fracture must be treated or prevented. Published reports of curettage and various forms of bone grafting, bone graft substitutes, treatment with autologous bone marrow, various bone void fillers, and placement of a variety of screws and hardware to "drain" the lesions appear frequently in the literature, but none of these treatments have been found to be superior to any other.
Preferred Margin for this Tumor
Intralesional
Outcomes of Treatment and Prognosis
Physicians should avoid operating on UBC whenever possible, and referral of recurrent or difficult cases to a musculoskeletal oncology center is indicated. Open curettage and bone graft have been reported with a recurrence rate of 40 to 45% due to difficulty of complete excision of the lesion. Surgeons must take care to avoid damage to the nearby growth plate which may result in growth arrest.
Special and Unusual Features
These lesions usually heal when the patient is skeletally mature, but a few persist into adulthood. The lesions grow in proportion to the growth of the bone they are in. Once the bone is finished growing, the UBC should also stop growing.