Summary
Prostate adenocarcinoma is both the second leading cause of cancer and the second leading cause of cancer death in North American males.
Complete Information on this Tumor
Prostate cancer is a relatively slow-growing type of cancer. Many men have it in their later years, but few of them actually die of it. Since it tends to effect elderly men, many men with prostate cancer will die of "natural causes" unrelated to the cancer. When prostate cancer affects younger men, it may take a more aggressive form and be rapidly spreading, and even fatal. Prostate cancer needs to be treated in different ways depending on the growth rate and stage of the tumor. Not all prostate cancers need aggressive treatment, and some may be safely monitored without treatment. When prostate cancer spreads to the bones, it cannot be cured, but there are many ways to slow and check the growth of prostate cancer.
Surgical treatment of metastatic prostate cancer in the skeleton is recommended for patients with debilitating skeletal lesions in patients with spinal cord compression who will benefit from the surgery.
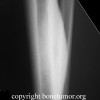
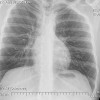
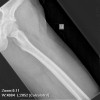
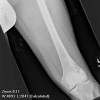
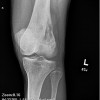
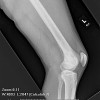
Other risk factors are a positive family history, and African-American males are twice as likely to develop the cancer than Caucasians. In advanced stages of prostate carcinoma, it can metastasize to various regions of the body, most commonly the lymph nodes and bone. The bones that are most commonly involved are vertebrae, sternum, pelvic bones, ribs, and femurs. The bony metastases are characterized by excess of abnormally dense bone. This indicates that there is increased bone turnover. Both osteoblastic and osteoclastic activities increase, but the relative amount of osteoblastic activity exceeds that of the osteoclasts, and bone formation is the net result.
Diagnosing prostate cancer usually begins with elevated serum PSA and/or prostatic acid phosphatase, or the palpation of nodules on a digital rectal exam. Diagnosis is typically confirmed by a biopsy guided by transrectal ultrasonography. PSA is also currently the most useful marker for assessing the level of bone involvement in prostate cancer. Diagnosis of bone metastases is accomplished by a bone scan. The problem with bone scans is that they are considered sensitive in the initial diagnosis, but the specificity is relatively low. They are also not suitable for monitoring short-term response to treatment. Other markers are currently under investigation to measure the amount of bone involvement. One such marker, pyridinoline cross-linked carboxy-terminal telopeptide of type I collagen (ICTP), is cleaved during type I collagen degradation which is indicative of bone turnover. The current thinking is that ICTP is more specific to bone than PSA, but further studies need to be done.
The actual mechanism by which metastatic cancer cells elicit osteoblastic reactions is not known. However, Koeneman et al have proposed that "in order to thrive in the bone environment, cancer cells must acquire 'bone cell-like' properties." It is believed that there are reciprocal cellular interactions between prostate cancer cells and bone stroma that result in proliferation of both prostate cancer and bone stromal cells. This interaction involves the participation of growth factors, such as TGF-ß, bFGF, and IGF on both bone and prostate, which is further modulated by the differentiating actions of bone morphogenetic proteins and PTH-related proteins. In the end, conditions are suited for osteoblastic growth, and the consequences are bone pain, inflammation, and increased risk for fractures.Also, vertebral tumors may compress the spinal cord and cause nerve damage. It is important to get a good feel for the level of bone involvement, because it has a significant impact on overall patient survival.
The current methods of treatment for prostate cancer are prostatectomy, radiation therapy, and hormone therapy. Hormone therapy can be accomplished by a few different methods. Orchiectomy and administration of estrogen are two options. Although 60-80% of patients with advanced prostate cancer improve following castration, there is an inevitable progression to a testicular androgen-independent state, in which adrenal androgens take over. There are also drugs that effect the pituitary gland directly, such as LHRH agonists, and some patients also receive antiandrogen drugs to block the effect of androgens produced from the adrenal glands producing a total androgen blockade.
Some patients with metastases often require additional treatment, such as second-line hormone therapy, which further suppress the production of androgens, or block their actions at the cancer cell itself. Other options are chemotherapy, radiation therapy, and bisphosphonates, which degrade osteoclasts, and prevent bone breakdown. Bisphosphonates are still under investigation for their effectiveness in metastatic prostate cancer. In cases in which the patient is in severe pain, administration of narcotics and a referral to a pain management specialist may be warranted.
It is recommended that patients with bone metastases should start androgen withdrawal therapy immediately upon diagnosis. However, hormone therapy does not provide a cure for the majority of cases of prostate cancer that have metastasized to bone. There are also many side effects of androgen ablation. Namely, decreased sexual functions, hot flushes, anemia, weight gain, and in the long run, bone loss and osteoporosis. A total androgen blockade has at best modest benefits.
The survival rate is projected at 8-10% at five years, and it has no advantage over orchiectomy at two years. Also, 60% of newly diagnosed patients with metastases die by 2 years. Routine periodic examinations and bone scans should be performed on a patient with metastatic prostate cancer. The goal is to prevent the progression of a metastasis to a pathological fracture.
Skeletal metastases are very common in prostate cancer. At autopsy, 84% of those with prostatic adenocarcinoma have skeletal metastases, while in 1982, of 20,000 new cases of prostate cancer, 21.5% of patients presented with clinical stage D (metastatic) prostate cancer. Skeletal metastases are also generally associated with poor prognosis. Only 23% of patients survived 5 years from initial diagnosis, and the 10-year survival rate is 10%.
As mentioned above, the most common sites for skeletal metastases are, in order of decreasing frequency, vertebrae, sternum, pelvic bones, ribs, and femurs.1 However, the most common sites for fracture are the medial cortex of the proximal femur and the vertebral bodies because these two sites are required to carry heavy loads.
Overall, the pathologic fracture rate from prostate cancer is relatively low compared to that of other metastatic cancers.9 The reason for this low rate is because of the bone forming osteoblastic reaction by the tumor. Even in those cases in which fractures do occur, the rate of healing approaches that of normal bone. Normal healing, in conjunction with effective radiotherapy and hormonal manipulation limits the need for surgical stabilization to only about one fourth of the patients who develop a pathologic fracture.
On the other hand, skeletal metastases that are predominantly osteolytic are rarely seen in prostate carcinoma.9 The authors feel that the osteolytic lesions that are seen in prostate cancer have a higher risk of fracture than osteoblastic metastases. That risk probably approaches that of other osteolytic metastatic cancers, such as breast cancer, lung cancer, and renal cancer. A patient with an impending pathological fracture can be treated with surgery, radiotherapy, chemotherapy, or hormonal manipulation.
The treatment of a pathologic fracture involves treating the neoplasm while also restoring structural stability; however, treatment of one may effect the treatment of the other. For example radiotherapy and chemotherapy may have adverse effects on the healing bone. For this reason, when postoperative radiotherapy is necessary, endoprosthetic replacements in the femur are the preferred method of surgical stabilization over osteosynthetic devices, because they do not require fracture healing. After surgical reconstruction, the wounds should be allowed to heal at least two weeks before starting radiotherapy or chemotherapy to reduce the risk of infection.
The oncologist and the orthopedic surgeon should jointly share postoperative follow-up, as about 25% of these patients will develop another bone metastasis requiring surgical stabilization. In a study performed by Wedin et al, 26 of 228 (11%) procedures for metastatic lesions of long bones led to failures necessitating reoperation. The overall failure rate of metastatic prostate cancer alone was 10%. Of the 26 failures, four were attributable to immediate failures, six to tumor progression, ten to nonunions, five to stress fractures of bone, and one to late dislocation of a humeral megaprosthesis and skin necrosis. Among 54 endoprostheses, only one (2%) patient had a reoperation, while among 162 operations involving osteosynthetic devices 22(14%) were failures. The reoperation rate in radiated fracture sites was 13% versus 10% in nonradiated sites. Five of the six patients who had reoperations for local tumor progression had not received radiotherapy to the fracture site, and eight of ten nonunions had been treated with radiotherapy. Also, all five patients who had a stress fracture had been treated with radiotherapy.9 All of this confirms that endoprostheses have a smaller failure rate that osteosynthetic devices, and that radiation may prevent tumor progression.
Surgical treatment of spine metastasis from prostate cancer is indicated for patients with motor weakness due to spinal cord compression. In one series, approximately half the patients treated with spine surgery for spinal cord compression improved at least one Frankel grade, which reinforces other data that show that decompression surgery combined with radiation is superior to radiation therapy alone in patients with metastatic epidural cord compression. (Patchell 2005)
Certain factors have a positive or negative influence on survival. Younger patients seem to have better survival than older patients. Extent of skeletal lesions (for example the number of lesions present on bone scan) is also predict survival. Solitary metastatic lesions have better survival than multiple lesions. Pathological fracture is a negative predictor of survival.
Treatment of pathological fractures is more difficult and has more frequent complications than treatment of normal fractures. In one series, there was a 9% rate of reoperation, especially peri-acetabular lesions treated with hip arthroplasty and reinforcement ring. These procedures have a very high rate of dislocation, as much as 25%.
For spinal cord compression, surgical decompression and postoperative radiation is superior to radiation alone in a randomized prospective study. (Patchell 2005)
Prostate cancer metastases tend to be blastic; that is, they tend to make the bones around them thicker and more dense, whereas many other types of cancer metastasis to the bones tend to be lytic, which means they tend to destroy and remove the bones around them. This means that pathological fractures are relatively uncommon in prostate cancer, and it is likely that a patient with prostate cancer in the spine will not suffer a pathological fracture. The metastatic deposits of prostate cancer in the spine can cause pain but there are many effective treatments available which the oncologist can use to eliminate the pain.
Prostate cancer is a relatively slow-growing type of cancer. Many men have it in their later years, but few of them actually die of it. Since it tends to effect elderly men, many men with prostate cancer will die of "natural causes" unrelated to the cancer. When prostate cancer affects younger men, it may take a more aggressive form and be rapidly spreading, and even fatal. Untreated prostate cancer is definitely fatal, but there are many ways to slow and check the growth of prostate cancer.
Even patients whose prostate cancer has spread to their bones enjoy a long survival, often several years, and occasionally many years.
Koeneman KS, Yeung F, Chung LW. Osteomimetic properties of prostate cancer cells: a hypothesis supporting the predilection of prostate cancer metastasis and growth in the bone environment. Prostate. 39(4):246-61, 1999
http://www.cancercenter.com/home/90/prostate/prostate2.cfm
Koga H, Naito S, Koto S, Sakamoto N, Nakashima M, Yamasaki T, Noma H, Kumazawa J. Use of bone turnover marker, pyridinoline cross-linked carboxyterminal telopeptide of type I collagen (ICTP), in the assessment and monitoring of bone metastasis in prostate cancer. Prostate. 39(1): 1-7, 1999 Apr 1. http://nurses.medscape.com/SCP/IIU/1999/v12.n03/u4503.fair/u4503.fair-01.html
http://apinet.site.yahoo.net/apinet/manofnewdiag.html
Walker RH. Pelvic reconstruction/total hip arthroplasty for metastatic acetabular insufficiency. Clin Orthop 1993;294:170
Murphy GP, et al. The national survey of prostate cancer in the United States by the American College of Surgeons. Journal of Urology 1982; 127:928.
Bostwick D. "Neoplasms of the Prostate." Urologic Surgical Pathology. Mosby-Year Book, Inc, 1997. St. Louis. Pp. 342-421.
Coyler, RA. "Surgical Stabilization of Pathological Neoplastic Fractures." Current Problems in Cancer. 10(3): 117-68, 1986 Mar.
Wedin R, Bauer HC, Wersall P. Failures after Operation for Skeletal Metastatic Lesions of Long Bones. Clinical Orthop 1999;358:128-139.
Harrington KD, Sim FH, Enis JE, et al. Methylmethacrylate as an adjunct in internal fixation of pathological fractures. J Bone Joint Surg 1976;58A:1047-1055.