Summary
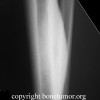
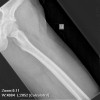
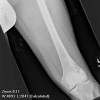
Bizarre parosteal osteochondromatous proliferation (BPOP) is a rare lesion that occurs most commonly in the hands and feet.
Complete Information on this Tumor
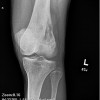
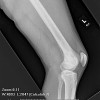
Bizarre parosteal osteochondromatous proliferation (BPOP) is a rare lesion that occurs most commonly in the hands and feet. This lesion grows rapidly and has aggressive features on imaging studies as well as confusion findings on histopathology, leading to many errors in diagnosis and potentially inappropriate treatments. The lesion is thought to be related to myositis ossificans, reactive periostitis and subungual exostosis. It was described in 1983 by Dr. Nora, and is sometimes called Nora's disease or Nora's lesion. Recently, this lesion has been shown to have an association with a specific translocation t(1:17)(q32;q21).
There is a history of a mildly painful mass that seems to increase in size over many weeks or a few months. There is usually no history of trauma. There may be stiffness of a nearby joint, or other mechanical symptoms.
Smith, Ellis, McCarthy, and McNaught Aust N Z J Surg
1996 Nov,66(11):781
Meneses, Unni, and Swee
Am J Surg Pathol 1993 Jul;17(7):691-7
Bandiera, Baccini, Bertoni Skeltal Radiol 1998 27:154-156
(J. H. Choi et al Skel Rad 2001 30:44-47)