Summary
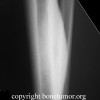
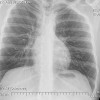
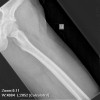
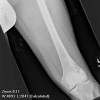
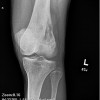
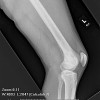
Most stress fractures can be readily identified based on the clinical history, plain x-ray findings, and MRI findings. However, in some cases there is a lack of an appropriate history, or the imaging findings are equivocal. In some cases stress fractures can be difficult to differentiate from infection, bone infarction, or malignant neoplasm.
Complete Information on this Tumor
Most stress fractures can be readily identified based on the clinical history, plain x-ray findings, and MRI findings. However, in some cases there is a lack of an appropriate history, or the imaging findings are equivocal. In some cases stress fractures can be difficult to differentiate from infection, bone infarction, or malignant neoplasm.
Some patients will present with pain and an early stress fracture without any history of prolonged activity or walking. Children may not be able to give a history that is sufficient for the clinician to consider stress fracture in the differential. Plain radiographs may also be misinterpreted.
Stress fractures are caused by repetitive episodes of mechanical loading, which results in bone strain. Strain is a unitless value that represents a change in the unit length per unit length of bone. The amount of injury caused by a given amount of strain increases with both magnitude and rate of application. During normal activities, a healthy bone is capable of targeted remodeling of injured areas. Both large loads applied over short periods or small loads applied repetitively without sufficient time for bone remodeling can cause stress fractures.
Stress fractures can be caused by extrinsic and intrinsic factors. Intrinsic factors include the type of activity or sport, training program, environmental factors, shoe characteristics and surface characteristics. Intrinsic factors include and bone structure, muscle dysfunction, joint flexibility, and foot shape. A cavus foot is associated with an increase of tibial stress fractures, where as a planus foot is associated with metatarsal stress fractures. (Ref: Foot Ankle. 1989 Aug;10(1):25-9. Combined effect of foot arch structure and an orthotic device on stress fractures. Simkin A1, Leichter I, Giladi M, Stein M, Milgrom C)
Common locations of stress fracture include the tibia, tarsal navicular, metatarsals, and fibula. Stress fracture location is based partly on the type of sport or activity. Endurance athletes are at increased risk of stress fractures in the proximal skeleton such as the femur, where as power athletes such as sprinters and weightlifters are more likely to have distal stress fractures in the tarsal bones or metatarsals.
Risk factors include repetitive, high intensity training, recreational runners averaging more than 25 miles per week, and participation in track, dance, basketball, and soccer. Women are at higher risk than men. Patients with low 25-hydroxyvitamin D levels are more prone to stress factors. Other risk factors include eating disorders, amenorrhea, osteoporosis, smoking, and consuming more than 10 alcoholic drinks per week.
The correct diagnosis can sometimes be made by reanalysis of the available imaging findings. Low-quality x-rays, MRI scans degraded by motion artifact, low field strength MRIs, and low quality MRI images should be repeated. For maximum diagnostic value, MRIs should combine T-1 and T-2 weighted images as well as short inversion time inversion recovery (STIR) as well as fat-suppressed T-2-weighted images. High-resolution multislice CT scan imaging focused on the area of interest can be very helpful in revealing fracture lines. Limiting the CT to the area of interest reduces radiation exposure. Bone scanning does not appear to increase diagnostic accuracy over the combination of claim x-ray, MRI, and CT scan. Biopsy is only rarely necessary. Careful attention to the interpretation of the biopsy is necessary due to the overlap between stress fracture histology and the histology of malignant bone tumors such as osteosarcoma.